Arthrosis of the knee joint (gonarthrosis)is a progressive chronic disease of the knee joint with damage, thinning and destruction of the cartilage (articular surface of the femur and tibia), as well as damage to the subchondral bone.It has been proven by studies (arthroscopy and MRI) that in addition to damage to the articular cartilage, menisci and synovial membrane are involved in the process.Gonarthrosis is one of the most common orthopedic pathologies.There are synonyms - osteoarthritis (OA), deforming arthrosis.This disease is an important socio-economic problem, because it is widespread and significantly worsens the quality of life of patients due to constant pain and, in addition, is a cause of high disability.
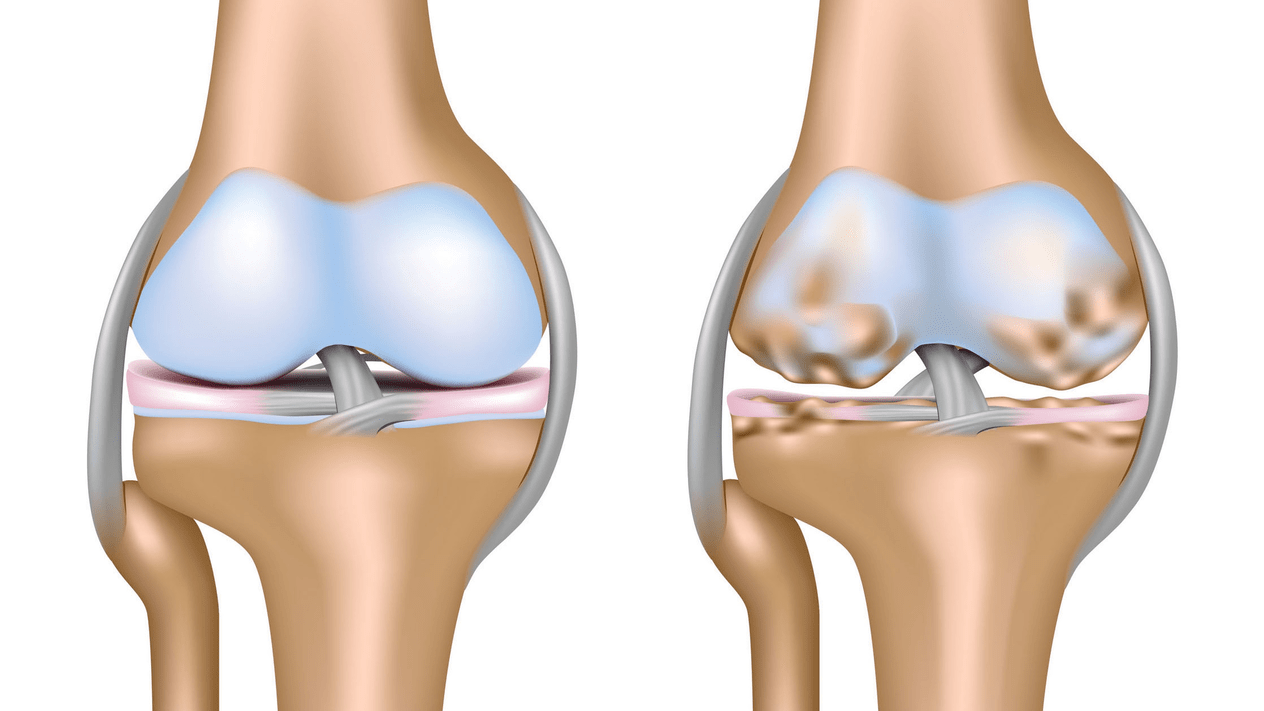
Until the mid-eighties of the last century, there was no unified definition of this disease.Until 1995, the osteoarthritis committee of the American College of Rheumatology characterized this disease as the result of mechanical and biological factors that lead to an imbalance between the degradation process and the synthesis of the extracellular matrix of articular cartilage.As a result, fragmentation and degeneration of fibers occurs, cracks, osteosclerosis and compaction of the cortical layer of subchondral bone are formed, osteophytes grow and subchondral cysts are formed.
Why does arthrosis of the knee joint occur?
Risk factors for arthrosis include:
- chronic traumatization (violation of physical activity, overweight);
- endocrine, inflammatory, metabolic and ischemic diseases;
- the presence of congenital or acquired disorders in the relationship, shape or organization of the articular end structure.
If you find similar symptoms, consult your doctor.Do not self-medicate - it is dangerous for your health!
Symptoms of arthrosis of the knee joint
Osteoarthritis of the knee joint is characterized by:
- gradual onset;
- mild pain in the joints when moving, especially when going up and down stairs;
- "tightening", stiffness and "starting pain" that occurs during the first step and decreases or disappears if the patient "diverges", after significant physical activity it resumes.
- the appearance of the knee remains the same.Sometimes there is a slight swelling or accumulation of fluid in the joint.At the same time, the knee increases in volume, swells, becomes flat, and restriction of movement and heaviness are felt.
A painful sensation
As the disease progresses, the pain becomes stronger, appears even with small efforts and walks for a long time.Localized along the anterior-inner surface of the joint.Prolonged rest usually helps the pain go away.
Limited mobility in the knee joint and characteristic irritation
With arthrosis, the range of motion of the joint may decrease, dryness may appear, and sharp pain appears when the leg is bent to the maximum.
Knee defect
The configuration of the joint changes, as if it is growing.
Synovitis
Synovitis of the knee joint is inflammation of the lining of the inner cavity of the joint.This disease manifests itself in the form of knee swelling, skin redness, and limited joint mobility.With the development of arthrosis, synovitis occurs more often, lasts longer and involves a large amount of fluid.
The last stage of gonarthrosis is distinguished by the fact that the pain becomes almost constant, causing anxiety not only when walking, but also at rest, and even at night, when the patient needs to find a comfortable position to sleep.Movement is more limited: it is difficult to fully bend and straighten the leg.Joints become deformed and increase in volume.Valgus (X-shaped) or varus (O-shaped) foot deformities are often observed.The gait becomes unsteady and swaying.In severe cases, crutches or crutches are required.
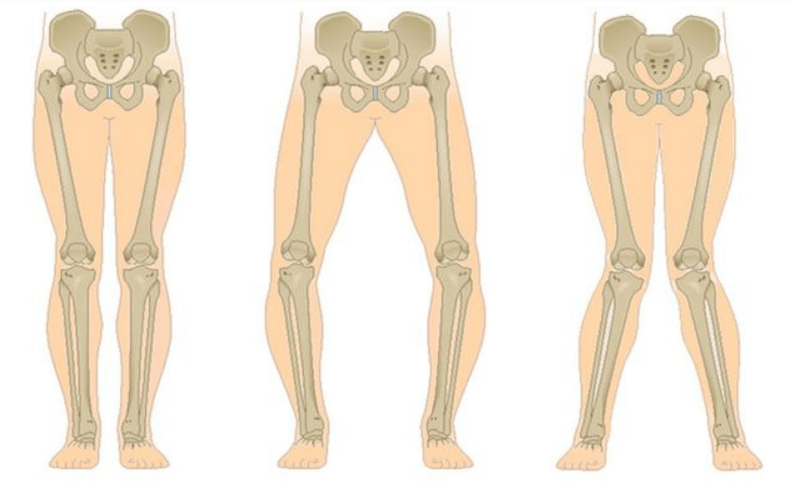
According to researchers, 76% of elderly people who complain of knee pain have radiographs showing gonarthrosis.According to statistics, women are more often affected by this disease, which is associated with hormonal changes after 45 years.
Pathogenesis of knee joint arthrosis
There are primary and secondary osteoarthritis.
Primary arthrosis of the knee joint
- Articular cartilage is constantly being destroyed and renewed;normally, this process is balanced.With age, cartilage renewal slows down and destruction begins to dominate, which is called the process of degradation or degeneration.A person's weight plays an important role, because with a mass of 70 kg in 20 steps we carry 700 kg on each leg (70 kg x 10 steps), and with a mass of 120 kg we already carry 1200 kg on each leg.Therefore, weak cartilage wears out faster;
- keep in mind: joints receive nutrients and are restored as they move;A sedentary lifestyle reduces metabolic processes, and the necessary elements do not reach the cartilage;
- There is controversial evidence regarding the role of heredity in the occurrence of this disease.If parents have arthrosis, then the likelihood of its occurrence in children increases;
- occurs as a result of autoimmune synovial inflammation.
Secondary arthrosis of the knee joint
- injuries (fracture, rupture of the meniscus and anterior cruciate ligament).Unfortunately, in any person, regardless of age, this injury leads to excessive pressure on the cartilage.Fracture of any part of the bone covered with cartilage is accompanied by the formation of an unevenness - "step".In this area, when moving, abrasion occurs and arthrosis forms;
- rheumatoid arthritis, Koenig's disease (osteochondritis dissecans), due to purulent inflammation of the joints (gonitis), etc.;
- regional vascular disorders;
- exudative-proliferative and chronic cicatricial adhesive processes in joints.
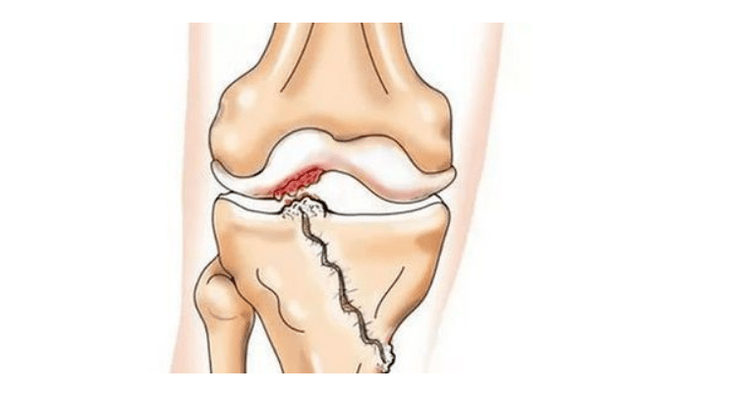
With arthrosis (osteoarthrosis), in addition to the progressive destruction of cartilage, loss of elasticity and shock-absorbing properties, bone is gradually involved in the process.Under load, sharp edges (exostoses) appear, which are mistakenly considered "salt deposits" - with classic arthrosis, no salt deposits occur.As arthrosis develops, it continues to "eat" the cartilage.Then the bones become deformed, cysts form there, all joint structures are affected, and the legs become bent.
In addition to the inside or outside of the knee, arthrosis can also affect the surface between the patella and the intercondylar groove of the femur.This option is calledpatellofemoral arthrosis.
The cause is usually subluxation, fracture, or lateralization of the patella.
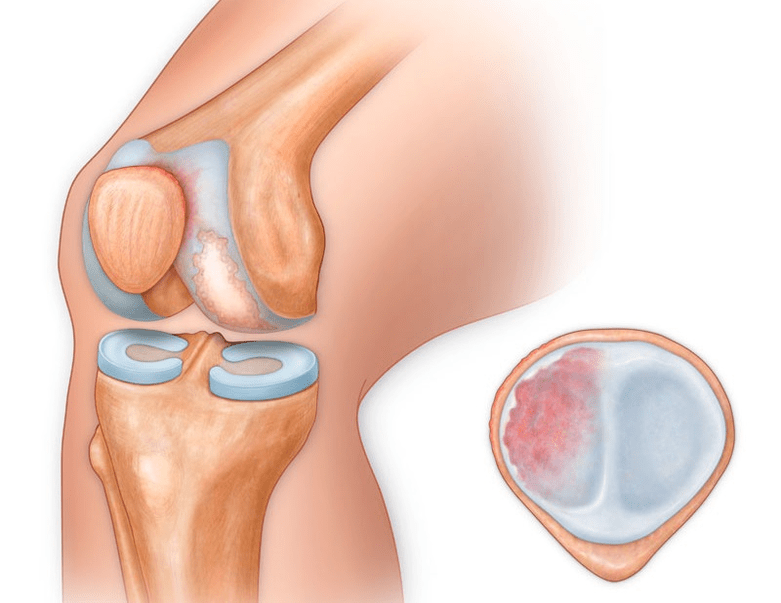
Classification and stages of development of arthrosis of the knee joint
Regardless of the cause, there are three stages of gonarthrosis, or arthrosis deformity of the knee joint.
Gonarthrosis, stage I
The first stage of the disease is characterized by major changes in the hyaline cartilage.Bone structure is not affected.Blood supply in intraosseous vessels and capillaries is disrupted.The cartilage surface becomes dry and loses its smoothness.If the disease is accompanied by persistent tense synovitis, then Baker's cyst develops (protrusion of the hernia of the joint capsule of the popliteal region).After significant pressure on the joint, dull pain occurs.There may be some swelling that goes away after resting.No deformation.
Gonarthrosis, stage II
In the second stage, the cartilage layer becomes thinner, and in some places is completely absent.Osteophytes appear along the edges of the articular surface.The qualitative and quantitative characteristics of the synovial fluid of the joint changes - it becomes thicker, more viscous, which leads to a deterioration in its nutritional and lubricating properties.The pain is more prolonged and intense, and a throbbing sound often appears when moving.There is little or moderate movement restriction and little joint deformity.Taking analgesics helps relieve pain.
Gonarthrosis, stage III
Lack of cartilage in the most affected areas, severe sclerosis (hardening) of the bones, many osteophytes and sharp narrowing or absence of the joint space.The pain is almost constant, the gait is disturbed.Mobility is very limited, and joint deformation can be seen.NSAIDs, physiotherapy and other standard methods of treating knee arthrosis are ineffective.
Types of gonarthrosis
Depending on the number of joints affected, unilateral and bilateral gonarthrosis are distinguished.
Complications of arthrosis of the knee joint
The most common complication in stages II and III is tendovaginitis of the thigh adductor muscle group.This is manifested by pain along the inner surface of the joint, which increases with movement.The cause is muscle imbalance and deformation.With a long-term decrease in range of motion, contractures develop.In addition, synovitis often occurs.
As a result of advanced gonarthrosis
Gonarthrosis affects the entire musculoskeletal system, disrupting the biomechanics of the spine and other large joints of the lower leg.This can cause herniated discs and arthritis in other joints.The second knee joint is loaded (if the disease is one-sided), because the patient saves the sick leg, transferring the weight to the other, healthy one.
Diagnosis of arthrosis of the knee joint
Instrumental diagnosis of arthrosis of the knee joint
In most cases, examination and x-ray of the knee joint in two projections (direct and lateral) is sufficient.Clinical data and images help determine the stage of the disease.
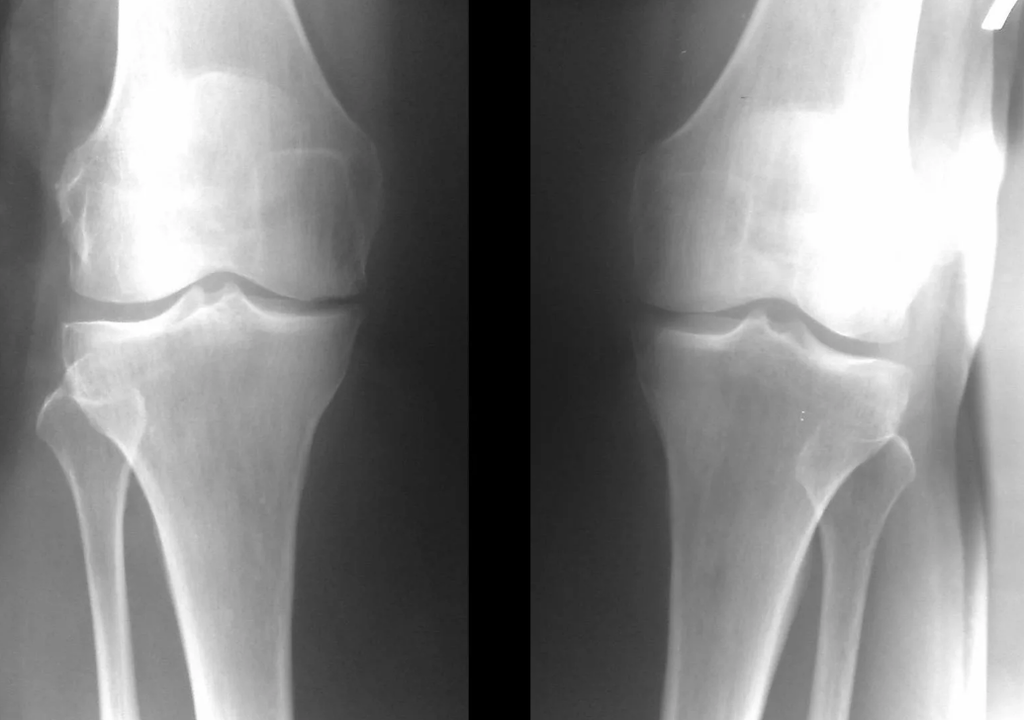
In the early stages of the disease, with minor changes in bone tissue, X-ray examination is not very valuable.At this stage, gonarthrosis can be diagnosed through arthroscopy.The accuracy of the method is very high;only its invasive nature and price can prevent it.
Ultrasound does not allow clear visualization of changes in articular cartilage and intra-articular structures.Using MRI, you can detect changes in the structure of bone, cartilage and soft tissue of joints, as well as subchondral bone, with an accuracy of 85%.Scintigraphy can be used to evaluate the metabolic activity of periarticular bone tissue.
Laboratory diagnosis of arthrosis of the knee joint
An increase in phosphorus and calcium content in dehydrated synovial fluid is evidence of the destruction of joint osteochondral tissue and the accumulation of degradation products.Blood is also checked - general analysis and erythrocyte sedimentation rate (ESR);determine the level of fibrinogen, urea and other biochemical parameters of blood and urine.
Is it possible to completely cure arthrosis of the deformed knee joint?
Gonarthrosis can be completely cured only in the early stages of the disease.
Which doctor treats deforming arthrosis of the knee joint?
A traumatologist-orthopedic specialist or a rheumatologist makes a diagnosis and prescribes treatment.
Treatment of arthrosis of the knee joint
Conservative — anti-inflammatory drugs, pain relievers, muscle relaxants, vascular, chondroprotectors, compresses, kinesiotaping, physical therapy, physiotherapy, orthosis.
Minimally invasive- para-articular blockade (Novocaine + drugs to relieve pain and inflammation), injection of artificial lubricant into the joint itself, plasma lifting.
Surgery - arthroscopy (low trauma method to treat intra-articular pathology and remove damaged structures), endoprosthetics.
Drug treatment (drugs for the treatment of arthrosis of the knee joint)
Conservative methods are most effective in the early stages of the disease.They help reduce pain and temporarily slow down the destruction of cartilage.In stage II, more effective methods are needed.The introduction of hyaluronic acid preparations into the joint cavity is used to reduce friction and trauma to the cartilage.There is no clear evidence for cartilage restoration, but it is good for lubricating surfaces."PRP therapy" (plasmolifting) is the injection of platelet-rich plasma into the knee joint, obtained from the patient's own blood by centrifugation.It nourishes the cartilage and promotes its recovery, because autoplasmic platelets contain many growth factors and cytokines that promote the regeneration of damaged tissue.
Surgical and endoprosthetic treatment
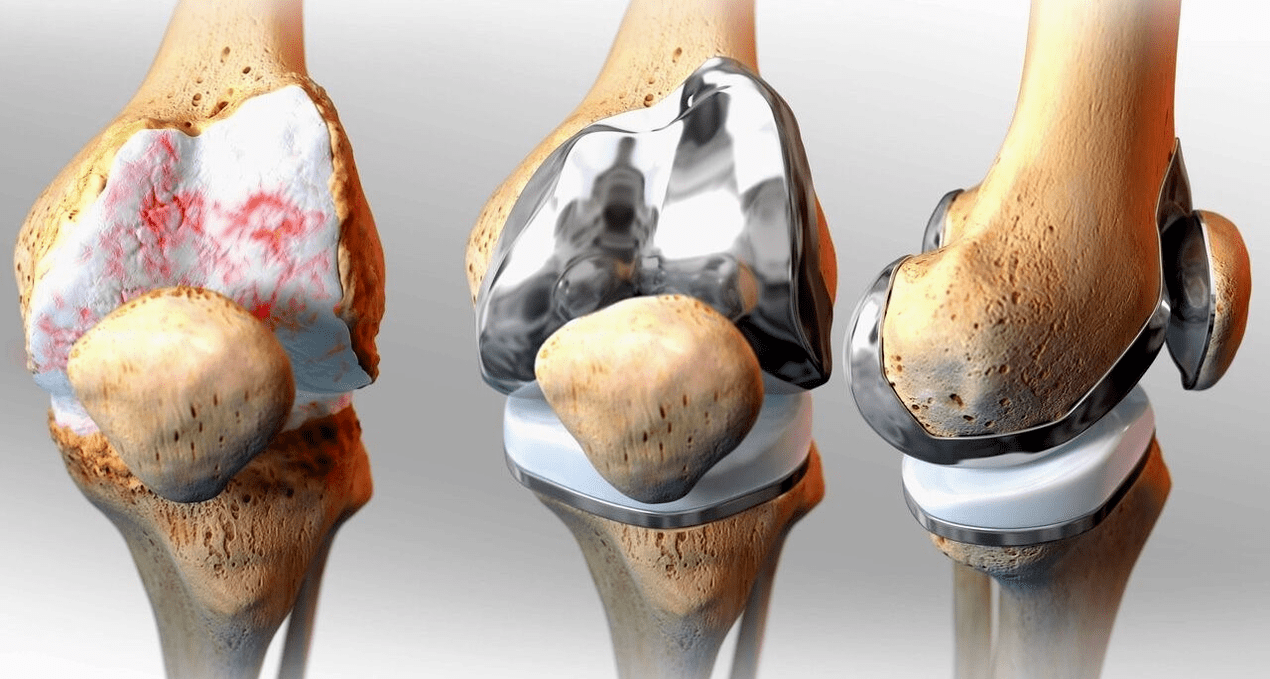
Endoprosthesis replacement is a common and effective surgical method for treating severe gonarthrosis, which allows you to maintain limb mobility and the ability to lead a full life afterwards.This is a high-tech operation that lasts about an hour and a half.In the postoperative period, long-term rehabilitation and development of the joint is necessary.After 25-30 years, when the artificial joint wears out, it needs to be replaced again.
Physiotherapy and kinesitherapy
Physiotherapy and kinesitherapy methods for the treatment of arthrosis of the knee joint are not effective.
Diet therapy
Diet is only necessary to maintain a normal body weight;there are no restrictions on the use of certain foods for gonarthrosis.
Do restrictions help with gonarthrosis?
For arthrosis of the knee joint, a para-articular block is used - an injection of medicine into the soft tissue around the joint.During the procedure, areas of inflammation and pain points near the joints are determined, the skin is treated with alcohol, and hydrocortisone with anesthetic is injected into these areas.
Therapeutic exercises for arthrosis
Therapeutic exercises are useful for patients suffering from gonarthrosis and for the prevention of this disease.Effective training:
- full flexion and extension of the legs, lying on your back;
- Raise your legs straight up while lying on your back.
Forecast.Prevention
You need to understand that if arthrosis begins to develop, then it must be treated immediately.If you are at risk for this disease, you can delay the start, for this it is recommended:
- reduce pressure on the knee joint;
- swimming - water relieves stress;
- massage the muscles of the lower legs and thighs themselves;
- avoid hypothermia and overwork;
- maintain a normal weight;
- stop smoking and alcohol;
- women wear comfortable low-heeled shoes;
- do physical therapy
Before starting therapeutic exercises, you should definitely consult with your doctor.Exercise is done at a slow pace.If pain or discomfort occurs during gymnastics, the exercise should be stopped.
It is necessary to use only effective drugs.Rubbing, compressing and other folk methods are ineffective;they do not act on the cause of the disease, but only help to distract from the pain.Avoid injury and overload - jumping, carrying heavy objects, standing for long periods or sitting in uncomfortable positions.This accelerates the development of the disease.
It is also necessary to diagnose and treat rheumatoid arthritis, gout and systemic diseases immediately.
What factors affect the long-term prognosis of knee arthrosis?
Prognosis depends on the stage at which the patient goes to the doctor and the correct therapy.The sooner you start the right treatment, the higher the chance of avoiding surgery.






















